pleurodesis
Download and print as a PDF
DownloadWhat is pleurodesis?
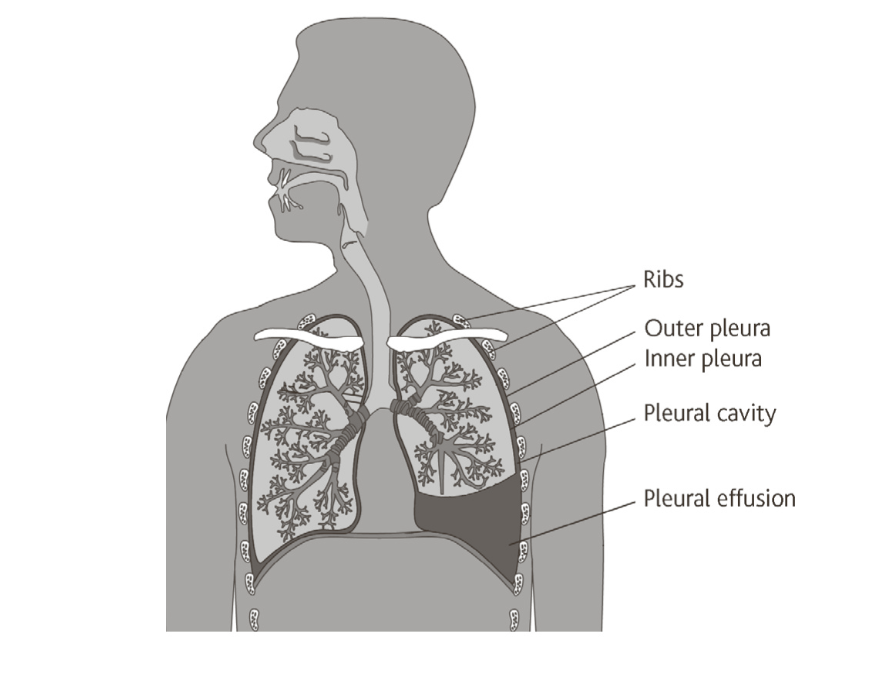
Pleurodesis is a procedure that aims to ‘stick’ the lung to the wall of the chest to prevent the re-accumulation of fluid (pleural effusion) or air (pneumothorax) which has collected in this space. This involves putting a substance into the space between your lung and chest wall (pleural space). The substance is put into the chest through a chest tube.
Who will be doing the procedure and where?
The procedure will be carried out by a qualified doctor with a suitable level of experience. Because this is a Teaching Hospital, the doctor performing the procedure may be supervised by a senior doctor. The procedure will take place in the procedure room in the Acute Medical Unit on Level 5 of the Thomas Kemp Tower at the Royal Sussex County Hospital.
How do I prepare?
You may be asked to have a blood test a few days before you come to hospital.
Please take any normal medicines including painkillers before you come in. If you are on blood thinning treatment such as Warfarin, Clopidogrel or injections your doctor should have arranged for these to be stopped in advance. If not please highlight this to the medical team.
You may also eat and drink as normal.
Most patients will be asked to arrive in the morning and be able to leave an hour or two after the procedure.
What happens during the procedure?
Initially a chest drain will be inserted to drain away the fluid or air that has collected in the pleural space; this procedure involves the following:
You will be asked to lie down on a bed where the doctor will use an ultrasound machine to show where best to insert the drain. The ultrasound enables the doctor to ‘look’ through the chest wall, it is painless and non-invasive. A cool gel is used on the skin to ensure good contact for the ultrasound probe.
Your skin will be cleaned and then a local anaesthetic will be injected to numb the area. The drain will then be inserted between the ribs in the anaesthetised area and connected to a tube and drainage bottle containing water. The water acts as a one way seal to allow air or fluid to drain out but not go back in to your chest.
Once your chest drain has drained completely, the Pleurodesis drug (which is usually sterile talc) will be put in to your chest through this drain. The drug is usually injected in a liquid form.
After the talc has been put into your chest, your drain may be closed off for about 1–2 hours. The drain will then be re-opened to allow drainage of any fluid or air to begin again. The chest drain is usually left in position for 72 hours but it may be left longer if the drainage of fluid or air continues. You will need to stay in hospital until the drainage is reduced and the doctor considers the drainage tube is no longer needed. Once the drain is removed the procedure is complete.
What happens afterwards?
A single stitch is sometimes needed to close the site where the chest drain was inserted. If so, it will be removed after seven days.
Will it hurt?
Sometimes Pleurodesis can cause some pain. We will give you some painkillers before the procedure to help with this. It is quite common to feel some discomfort during the procedure. If this happens, please let the nurse or doctor know so that we can give you more painkillers.
How will the drain be attached?
We use a stitch to tie the drain in and an adhesive dressing on the skin; however, please move carefully as drains can still be pulled out.
How will the drain be removed?
This is straight forward and is usually done by a nurse. Once all the dressings are removed the drain will be gently pulled out. You may be asked to hold your breath in a special way when this is done. It can be uncomfortable but only lasts a few seconds.
Are there any risks during the procedure?
Most patients undergo Pleurodesis without any major problems; however, like all medical treatments it does have some risks:
Sometimes patients experience chest pain from Pleurodesis. Painkillers are given as needed to help relieve this.
Some patients experience fever for the first day or two after the procedure. This is usually controlled with Paracetamol and is short-lived.
Sometimes Pleurodesis can cause breathlessness due to too much inflammation in the lung. This usually settles down over a few days with oxygen treatment, although very, very rarely (about 1 in 1000) it can be serious.
All treatments that require a tube in the chest carry some risk of causing infection. This happens in about 1 in 50 (2%) of patients. Should this happen it usually settles with antibiotic treatment although it may lead to a longer hospital stay.
Useful contact numbers and website
Acute Medical Unit: 01273 696955, extension 3435.
Respiratory Secretaries: 01273 696955, extension 3106/3107).
District Nurses: 01273 885000.
Website: www.patient.co.uk.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information here is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Publication Date: September 2014
Review Date: January 2023


