After your ankle operation for when you can partially weight bear
Download and print as a PDF
Download- How much should I move and exercise my injured foot?
- How can I prevent swelling?
- When should I wear the boot?
- Can I have some pain relief?
- Can cold packs help?
- What’s the best way to wash?
- How can I manage stairs with my crutch?
- Will I have on going physiotherapy?
- Initial Exercises to do 3 to 4 times a day.
- Frequently asked questions:
- Who can I contact if I have any other questions?
How much should I move and exercise my injured foot?
Early weight bearing (putting weight through your injured foot) has been shown to help increase the speed of healing. You should not be mobilising (moving around) or have your ankle lowered to the floor for very long for two weeks after your surgery to allow the swelling to go down and the wound to heal.
Your wound will be checked and as long as it has healed then you can start to mobilise more on crutches. Be aware that if you are on your feet for long during the day or do too much your ankle will swell and this can impact on the healing of your injury. The ideal is little and often.
Try to walk as normally as possible partial weight bearing on the leg as this will help with your recovery. Partial weight bearing means that you should only be putting half of your body weight on your operated foot. You can aim to keep your heel off the floor to help with this.
How can I prevent swelling?
You must keep your foot elevated, ideally above the level of your hips, whenever you are not moving for the first two weeks. If the ankle is not elevated, the wound may not heal properly and potentially risk an infection so this is very important.
When should I wear the boot?
The boot should be worn whenever you are moving, even around the house. It is for protection and support. You can remove the boot at night when sleeping and when resting and when you are doing your exercises.
Can I have some pain relief?
You will be given pain killers to take home. You should take this on a regular basis to begin with to help you move and do the exercises.
Can cold packs help?
A cold pack (ice / frozen peas) can provide short term pain relief right after the operation but this must be in a waterproof bag as you must not get the dressings wet. Apply it to the ankle for up to 15 minutes, every few hours. Make sure that the ice is never in direct contact with the skin. This may not have a significant effect while the bandages are on but will help more when the dressings are removed after two weeks.
What’s the best way to wash?
The most important thing is to keep the dressings dry until the wound has healed and the dressings are removed.
Options for washing (depending on facilities) are a strip wash at a sink or a shower. You can put a waterproof bag over your leg or you can buy a cover called a Limbo from the internet.
Go to www.limboproducts.co.uk.
How can I manage stairs with my crutch?
Going Up: ABC (Able leg, Bad leg, Crutch to the same step)
Going Down: CBA (Crutch, Bad leg, Able leg to the same step)
Remember: Only put half of your body weight on your operated or ‘bad’ leg.
Will I have on going physiotherapy?
You will be referred to an NHS Outpatient physiotherapy department close to where you live. You will be seen by your consultant first usually 6 weeks after your operation.
Once they have allowed you to fully weight bear (put all your body weight on your operated leg), they can refer you on for a physiotherapy appointment. You will then continue to have regular physiotherapy appointments to help with your rehabilitation and help you to return to normal activities.
If you have private healthcare then we can give you a copy of your operation notes to take with you to your first appointment.
Please follow the management/rehabilitation plan shown below:
| Weeks since injury | Rehabilitation plan |
| 0-6 | Wear boot all the time when mobilising. Walk with crutches partially weight bearing. Perform exercises below to help with range of movement. |
| 6-8 | You will have an orthopaedic follow up appointment around 6 weeks after the operation and another x-ray to check how the bone is healing. You should then be able to begin fully weight bearing still in the boot. You will also begin to see the Physiotherapist. |
| 8 -12 | You will start to progress your mobility and wean out of the boot slowly. Your Physiotherapist will be able to guide you back to your normal daily activities as your rehab progresses. |
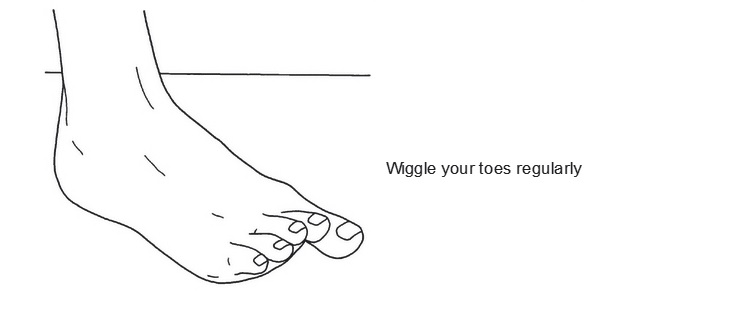
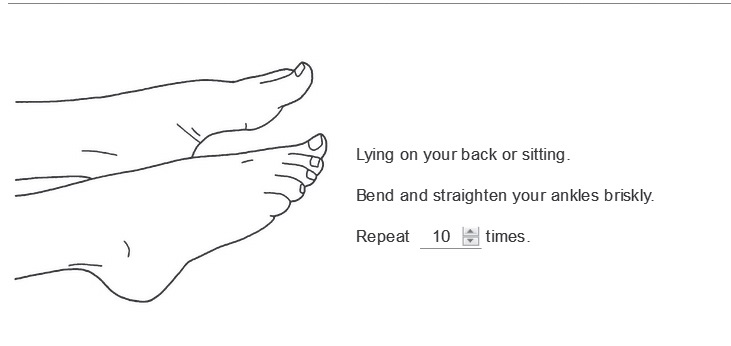
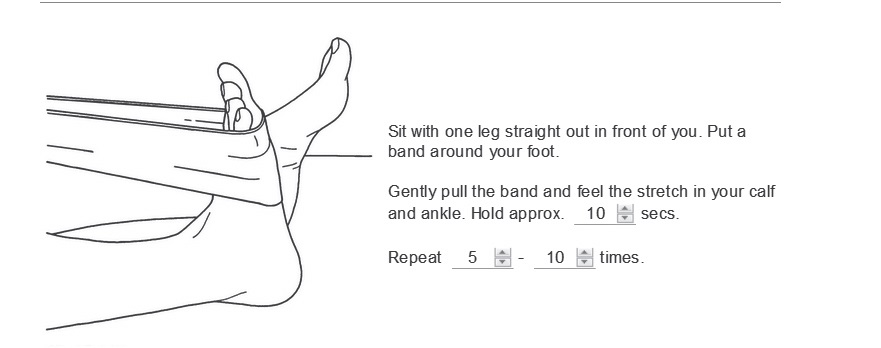
Initial Exercises to do 3 to 4 times a day.
Frequently asked questions:
When can I return to work?
This depends on your job and what you do. If your job role involves moving around and / or commuting to work it may not be possible for you to return to work until you are fully weight bearing, this will be a minimum of 6 weeks. If possible you should talk with your employer and / or occupational health department to help with your return to work.
Your progress will be monitored by your consultant and physiotherapist who will help guide you to return to work as appropriate.
When can I return to driving?
You need to be able to perform an emergency stop without significant pain to ensure you are safe to drive.
If the fracture is on your right foot and you drive a manual vehicle you will not be able to drive for at least 8 to 10 weeks as you will still be in a boot.
If your fracture is on the left and you drive an automatic vehicle you may be able to drive before this. However you should get advice from individual insurance companies before returning to driving. It is also recommended that you try on a quiet road with someone sitting in the car with you on your first attempt.
When can I return to exercise?
You will begin physiotherapy once you are able to fully weight bear; this is likely to be from 6 weeks onwards.
The physiotherapists will progress you out of your boot and work on your strength, range of movement and balance. They will tailor a home exercise programme for you and guide you back to the activities or sports you enjoy as your rehab progresses.
Who can I contact if I have any other questions?
You can speak to a physiotherapist by contacting 01273 696955 and ask for bleep 8375 before your first appointment.
This information is intended for patients receiving care at Brighton and Haywards Heath.
The information in this leaflet is for guidance purposes only and is in noway intended to replace professional clinical advice by a qualified practitioner.
Publication Date: July 2020
Review Date: January 2023


