Pelvic floor repair with or without vaginal hysterectomy and/or Sacrospinous Fixation
Download and print this article
Download- What are these operations?
- Why do I need this kind of surgery?
- What can I expect before the operation?
- What does the operation involve?
- What are the risks?
- What can I expect after the operation?
- What about going home?
- What about follow up?
- Are there any alternatives to this kind of surgery?
- Who can I contact with any concerns or questions?
What are these operations?
Surgery for prolapse of the vaginal wall.
The repair may include:
- Anterior repair, to correct prolapse of the bladder.
- Posterior repair, to correct prolapse of the rectum.
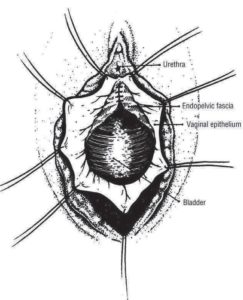
Anterior repair
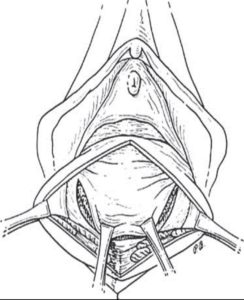
Posterior repair
Surgery for prolapse of the uterus.
There is a choice between removal of the uterus (vaginal hysterectomy) and supporting it (sacrospinous hysteropexy).
This can be managed with:
- Vaginal hysterectomy. In some instances, the top of the vagina might be very weak. In these cases, supporting the top of the vagina by stitching it to a ligament (band of fibrous tissue) in the pelvis is also needed. This is known as sacrospinous fixation.
- Sacrospinous fixation of the cervix, also known as sacrospinous hysteropexy.
Surgery for prolapse of the vaginal vault.
Patients who previously had a hysterectomy may also have prolapse of the top of the vaginal vault. This may need sacrospinous fixation of the vaginal vault.
The selection of the actual form of surgery will depend on the nature and extent of the prolapse you have and your doctor will discuss this with you.
These operations can be carried out under general or regional, such as spinal anaesthesia. An isolated anterior or posterior repair can be done under local anaesthesia, in selected patients
Why do I need this kind of surgery?
This kind of surgery is done to repair pelvic organ prolapse. This refers to slipping down of the vagina, the uterus and / or the top of the vagina after hysterectomy.
This prolapse is caused by weakness of the supports that keep the vagina and uterus in place. This weakness can result from a number of factors, such as child bearing, going through the menopause or weak ligaments and muscles. The condition can cause a sense of bulge, discomfort, urinary and bowel problems and sexual difficulties.
What can I expect before the operation?
At your pre op assessment and on your admission day, the nurse will go through your hospital stay and explain your operation.
Please do let us know about any concerns you have or if there is any information you think we should know about that will make your stay with us more comfortable.
You will need to make arrangements for your family, children or any other commitments that you have prior to coming in to hospital and to cover the length of your recovery.
You will see an anaesthetist and the doctor performing the surgery before you go to theatre. It is not unusual to feel anxious; the nursing staff will gladly discuss how you are feeling and talk you through your emotions.
If you have not already signed the consent form in outpatients, when the operation was booked, the doctor will go through it with you before you go to theatre. If you have not completed a quality of life questionnaire, you will be given one to complete.
You will be asked for permission to enter your data on the national database for continence and prolapse surgery. This is a quality control measure to compare the safety and effectiveness of such procedures at the hospital against other units in the country.
Completing a frequency volume chart and quality of life questionnaire at follow up will enable assessing the benefit of surgery for you.
What does the operation involve?
The operation is done through the vagina. A cut is made in the wall of the vagina through which the bladder and / or rectum are lifted up and secured in place with sutures.
If the uterus is to be removed, this is carried out through the cut in the vaginal wall. If sacrospinous fixation is to be carried out, dissection is extended to reach the sacrospinous ligament, where sutures are placed to support the top of the vagina or the cervix.
The vaginal wound is then closed with sutures. A gauze pack may be left in the vagina. A catheter may be inserted in the bladder, to save you the need to go to the toilet until you are mobile.
What are the risks?
There are risks with any operation but these are small. The main risks associated with these operations are:
Common risks:
- Initial difficulty in passing urine. This is usually managed by leaving the catheter to drain the bladder for longer. You can go home with a leg bag to drain the catheter for few days. This leg bag will not be visible to others and you can walk as normal. You go to the toilet from time to time to empty it.
- Postoperative pain.
- Urinary tract infection, which may need antibiotics.
- Wound infection, which may need antibiotics.
- Wound bruising and delayed wound healing.
Uncommon risks:
- Damage to the bladder and / or bowel, which will be repaired at the time of the operation. If such injury is not identified and repaired at the time, there is a risk of fistula, which entails an open wound between the bladder and / or bowel and the vagina. This is extremely rare.
- Venous thrombosis and pulmonary embolism (blood clot in leg / lung). The occurrence of these clots is reduced by elastic stockings and injections that thin the blood to prevent clots.
- Whilst the operation may improve the sense of bulge, there is a small chance that urinary, bowel and / or sexual problems may persist. It is hoped however they will at least improve to some degree.
- Unmasking of stress incontinence of urine that was hidden by the kink of the urethra, associated with prolapse. This will need assessment and will be managed by pelvic floor exercises. It may require an operation to improve continence.
- The operation may fail or prolapse may recur with time.
- Haemorrhage requiring blood transfusion.
- Return to theatre e.g. because of bleeding.
In order for you to make an informed choice about your surgery please ask one of the doctors or nurses if you have any questions about the operation before signing the consent form.
What can I expect after the operation?
As you come round from the anaesthetic, you may experience episodes of pain and / or nausea. Please let the nursing staff know and they will assess you and take appropriate action.
You may have a pack in the vagina and a catheter in the bladder to save you having to go to the toilet.
You will have a drip to give you fluids, though you will be able to eat and drink. It is not unusual to experience lower back pain and a feeling of fullness in your bowel and generalised discomfort when sitting. We use a pain score to assess your pain 0 to 10 [0 = No Pain, 10 = Very Strong Pain].
Your nurse will be checking your blood pressure, pulse, respiration and temperature and monitor any vaginal bleeding. S/he will also ask you to move from side to side and to do leg and breathing exercises once you are able to. This will help prevent any pressure damage, DVT (deep vein thrombosis) or chest infection.
Day 1 after the operation:
The drip, pack and catheter are usually removed the next day. The nursing staff will assist with washing as necessary and encourage early mobilisation. We would normally expect you to sit out of bed and begin to walk around the day after your operation.
You will be able to go home when you are passing urine without diffi-culty. This varies according to the actual operation and from patient to patient. Some may go home on the same day. Some may go home on day 1 whilst others may stay for 2 to 3 days.
You may be asked to pass urine in a jug and will have a scan to measure how much urine is left in the bladder.
Day 2 after the operation:
You will be able to shower and mobilise around the ward on the second day of your operation. It may be painful to open your bowels at first, we will give you mild laxatives to soften your stools and prevent constipation and straining.
What about going home?
You will be seen and assessed the following day to check on your recovery and decisions will be made about your care, this information will be shared with you. You may then be able to go home. Please feel free to ask questions about your operation and recovery at any time.
The average length of stay following this kind of surgery is 1 to 2 days. Patients having anterior or posterior repair only may go home on the day, especially if they have this repair under local anaesthesia.
As you physically recover from your operation, the nursing team will discuss your convalescence. To ensure you have a good recovery you should take note of the following:
Rest: During the first two weeks at home it is common to feel tired, exhausted and emotional. You should relax during the day, gradually increasing the number of things you do each day. Avoid crossing your legs when you are lying down.
Vaginal bleeding: You can expect to have some vaginal discharge / bleeding for few days after surgery. This is like a light period and is red or brown in colour. Sanitary towels should be used not tampons to reduce the risk of infection.
Stitches: The wound in the vagina will be closed by dissolvable stitches.
Housework:
Weeks 1 to 2: We recommend that you do light activities around the house and avoid any heavy lifting (not more than 1.5kgs in each hand).
Weeks 3 to 4: We recommend that you gradually introduce lighter house hold chores such as dusting, washing up, making beds and ironing. You may begin to prepare food and cook remembering not to lift any heavy items.
Weeks 4 to 6: By this time you should resume normal daily activities, but continue to refrain from straining for 3 months after surgery, to ensure good tissue healing.
Exercise: Exercise is important and it is advisable to go for short walks each day, increasing the distance gradually. You should avoid straining or heavy exercise for 3 months, to ensure good tissue healing. You may return to light exercise such as gentle cycling and swimming after 4 to 6 weeks. You will be able to manage the stairs on your arrival home. We encourage you to do pelvic floor exercises.
Diet: A well balanced nutritious diet with high fibre content is essential to avoid constipation. Your bowels may take some time to return to normal after your operation and you may need to take laxatives. You should include at least 5 portions of fruit and vegetables per day. You should aim to drink at least 2 litres of water per day.
Sex: You should usually allow 4 to 6 weeks after the operation before having sex to allow the vaginal wound to heal. If you experience vaginal dryness, you may wish to try a vaginal lubricant from your local pharmacy. If after this time you are experiencing pain or any problems with intercourse then you should see your GP.
Returning to work: This will depend on the nature of your work. If you work in an office based environment, you will need 4 to 6 weeks off work. If your work involves lifting and exertion, you will need 3 months off work. The hospital doctor will provide a sick certificate for this period.
Driving: It is usually safe to drive after 12 weeks but this will depend on your level of concentration, ability to perform an emergency stop and your car insurance policy.
What about follow up?
You will be invited for follow up, usually about 12 weeks after surgery.
During this follow up appointment, your symptoms will be reviewed, your quality of life will be checked and you will be examined, to assess wound healing.
If you have problems before this, you can contact your doctor or contact the hospital to bring the appointment forwards.
Are there any alternatives to this kind of surgery?
You will have been offered a vaginal pessary before being offered surgery.
Alternative procedures include:
- Operations through abdominal or laparoscopic route. These operations include sacrocolpopexy for patients who had previous hysterectomy and sacrohysteropexy for patients who still have their uterus and wish to keep it.
These can be discussed with your doctor.
Who can I contact with any concerns or questions?
You should contact your doctor or the hospital if you notice increased temperature, wound swelling and / or pain, smelling discharge either from the front passage, blood in urine or motion, abdominal distension and / or failure to open your bowel.
To contact the Gynaecology department please use one of the telephone numbers below.
Princess Royal Hospital, Horsted Keynes Ward: 01444 441881 Extension 5686
Royal Sussex County Hospital, Level 11: 01273 523191 Extension 4013
Urogynaecology Unit at Lewes Victoria Hospital: 01273 474153 Extension 2178
Useful links:
Your Pelvic Floor website: Anterior Vaginal Repair
Your Pelvic Floor website: Posterior Vaginal Wall & Perineal Body Repair
Your Pelvic Floor website: Recovery Guide After Vaginal Repair Surgery/Vaginal Hysterectomy
Your Pelvic Floor website: Sacrospinous Fixation/Illeococcygeus Suspension
www.patient.co.uk: Genitourinary Prolapse
Royal College of Obstetricians and Gynaecologists: Pelvic floor repair operation
Royal College of Obstetricians and Gynaecologists: Vaginal hysterectomy
This leaflet is intended for patients receiving care in Brighton & Hove or Haywards Heath.
This patient information leaflet was prepared by Dr. Sharif Ismail, Consultant Subspecialist Urogynaecologist.
This information leaflet has been approved at the Clinical Governance and Safety and Quality Meetings of the Department of Obstetrics and Gynaecology as well as Brighton and Sussex University Hospitals NHS Trust Carer and Patient Information Group (CPIG).
Ratified April 2017 Women’s Safety and Quality Committee.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Publication Date: May 2021
Review Date: February 2024

