Hallux rigidus correction
Download and print as a PDF
DownloadWhat is hallux rigidus?
Arthritis (wear and tear) is the most common cause of hallux rigidus. The arthritis develops in the joints at the base of the big toe, and is caused by the wearing out of the joints surfaces. This can develop in people of all ages.
With this condition you can develop inflammation and stiffness, leading to reduced mobility of the big toe causing pain in the joint and the ball of the foot.
Treatments that can help reduce pain in the toe and ball of the foot include orthotics and hard soled shoes. The aim is to off load the pressure on your big toe. Steroid injections are also available and can help to reduce inflammation.
Surgical intervention is often considered once non-surgical treatments are no longer helping to alleviate your pain and daily activities become difficult to manage.
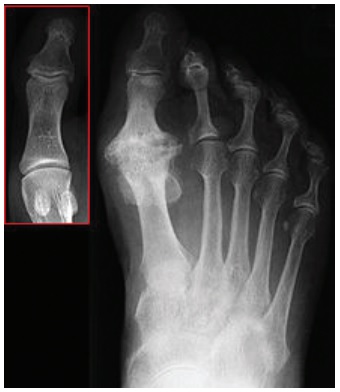
Hallux rigidus, before and after surgery
What happens during surgery?
The surgery performed for hallux rigidus is called a cheilectomy. The aim of the surgery is to reduce pain and prevent the arthritis from getting worse.
With a minimally invasive cheilectomy a 3mm cut is made into the side of the big toe. Through this cut the surgeon is able to remove the ridge of bone by using a very small drill called a burr. This is done under x-ray guidance.
With an open cheilectomy, a 5cm cut is made into the side of the toe. There are a number of reasons why a minimally invasive technique is preferred by some surgeons; a possible reduction in the risk of infection and pain, a quicker recovery period due to reduced tissue trauma and a reduction in joint stiffness.
What happens after surgery?
You will have your surgery at the Sussex Orthopaedic Treatment Centre (SOTC). This is usually done as day case surgery using either; regional anaesthesia (regional nerve block) that numbs your leg, or a general anaesthetic.
You will be able to put your full weight through your foot immediately after your surgery. You will be given an orthopaedic flat shoe and a pair of crutches to help with walking. The crutches can be used for the first few days after surgery. Patients usually find that within 3-4 days they feel confident enough to walk without the aid of crutches. We would encourage you to discard the crutches in the first week after your surgery.
You will be told by the recovery staff to remove the orthopaedic flat shoe and to take down the bandages after 2 days. Please leave the adhesive dressing on for a further 5 days. Once the adhesive dressing is removed you are then able to get your foot wet.
The recovery staff will also ask you to start moving your toe joint immediately once you remove your bandages. The slower you are to start moving the toe joint the longer the recovery period.
After your surgery we advise you to elevate your leg as high as you are able during the first couple of days when at rest and to apply ice to your foot. Elevation and icing of the foot will help to reduce swelling. The swelling can be expected to last for between for 3-6 months.
Four weeks after surgery
At 4 weeks you will have a follow up appointment with Mr Vernois. An x-ray will be taken and this will be reviewed. Mr Vernois will assess the range of movement in your joints and you will be able to ask any questions you may have. You can start to drive and resume low impact sports after this appointment.
Three months after surgery
You will have an appointment with Mr Vernois and an x-ray of your foot will be taken and reviewed. You will then be discharged from his care.
High impact sport can be resumed after this appointment.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The here is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Publication Date: February 2019
Review Date: December 2022


