fetal heart monitoring during labour
Download and print as a PDF
Download- What is fetal heart monitoring?
- How is it done?
- Why do I need fetal heart monitoring?
- What are the risks of fetal heart monitoring?
- What are the benefits of fetal heart monitoring?
- What other options are there?
- What happens if I choose not to have any fetal heart monitoring?
- Where can I find further information?
What is fetal heart monitoring?
Most babies go through labour and are born without any problems. But there are a few babies who have difficulties and the best way of finding out when a baby is having problems is to listen to every baby’s heartbeat regularly during labour. This is called fetal heart monitoring.
Your baby’s heartbeat can be monitored in two ways:
- At regular intervals, this is called intermittent auscultation.
- Continuously by electronic fetal monitoring (EFM).
When monitoring the baby’s heartbeat, the midwife will check your heartbeat by taking your pulse to make sure they can tell them apart.
How is it done?
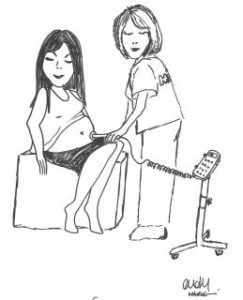
Intermittent auscultation can be done in two ways
- By using an instrument like an ear trumpet called a Pinnard stethoscope.
- By using a hand held ultrasound machine called a Doppler, your midwife may also call it a Sonicaid.
You may have seen your community midwife use these during pregnancy. The baby’s heartbeat is normally monitored every 15-30 minutes during the first stage of labour and more often during the second stage of labour or the ‘pushing’ stage.
Please note. The only way your baby’s heartbeat can be monitored at home or in water is with a pinnard stethoscope or doppler. If a problem is detected you may advised to have continuous EFM which will mean going into hospital.
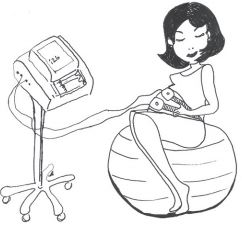
Continuous electronic fetal monitoring (EFM) can also be done in two ways
- By fastening two receivers around your abdomen (tummy). One receiver monitors the baby’s heartbeat while the other receiver monitors the frequency of the contractions.
- By fastening one receiver around your abdomen to monitor the frequency of the contractions. The other receiver, called a fetal scalp electrode (FSE), is on the end of a very small wire which is passed up the vagina (the same as an internal examination) and fastened on to the baby’s head by a very small clip.
- A FSE does not harm the baby although you may notice a small graze on the baby’s head after birth. The electrode can then pick up the signals of the baby’s heartbeat more easily because it is directly attached to the baby. This electrode stays in place until the baby is born.
The monitor records your baby’s heartbeat as a pattern on a piece of graph paper which is called a cardiotocograph (CTG) or a ‘trace’. The midwife and the doctor will interpret the trace to get an idea of how the baby is coping with labour. They will be able to explain their findings to you.
Why do I need fetal heart monitoring?
During contractions blood can not get through to the placenta (afterbirth) so easily and your baby may get less oxygen than usual. This is normal and most babies cope with no problems. But if the baby is not coping, the pattern of the heartbeat usually changes and this could mean that the baby needs to be born more quickly.
If you are healthy and have had a trouble-free pregnancy then the recommended method for fetal heart monitoring is using the pinnard stethoscope or hand-held doppler. Current research does not support the need for EFM even as part of the admission procedure.
If you have a health problem or any factor relating to your pregnancy that put you or your baby at increased risk, then the recommended method for fetal heart monitoring is continuous EFM.
Examples of problems include:
- Diabetes.
- Infection.
- Pregnancy induced hypertension (raised blood pressure due to the pregnancy).
- Problems with your heart or kidneys.
- Your pregnancy is more than 42 weeks.
- You are having an epidural as pain relief.
- You have had any bleeding from your vagina before or during labour.
- Your labour has been induced or accelerated.
- You have previously had a caesarean section.
- You have a multiple pregnancy.
- Your baby is small or premature.
- Your baby is a breech presentation (going to be born bottom first).
- When the midwife using intermittent auscultation detects a problem.
- If when the waters break they are not clear in colour.
What are the risks of fetal heart monitoring?
Being attached to the monitor for continuous EFM can limit your ability to move, however you will still be able to adopt a variety of positions.
What are the benefits of fetal heart monitoring?
When the midwife/doctor detects a problem with your baby’s heartbeat you may be offered a test called fetal blood sampling (FBS). This is a procedure which involves taking 1 or 2 drops of blood from your baby’s head (via an internal examination through your vagina). This blood is tested for levels of oxygen to show how well your baby is coping with labour. The test takes 10-20 minutes and is a more accurate picture of the baby’s condition. This test does not harm the baby but may leave a small graze on the baby’s head once born.
If the baby is coping well then it is less likely that you will require delivery by caesarean section, forceps or ventouse (suction cup). If the baby is not coping well then the doctor will discuss a plan of care with you.
What other options are there?
Not to have any fetal heart monitoring.
The other indications that a baby is coping well in labour include
- The baby’s movements, but these can be difficult to observe during labour because the woman’s abdomen will be tense during contractions.
- The colour of the liquor (your waters) should be clear. However the waters break (naturally or forced), if they are not clear this alone does not necessarily mean that the baby is distressed, in these cases we would strongly recommend EFM to achieve closer observation of the baby.
What happens if I choose not to have any fetal heart monitoring?
The kind of monitoring you have while you are in labour is up to you. The majority of women like to be able to hear their baby’s heartbeat while others find it worrying.
If you are reluctant to have any fetal heart monitoring it would be best to discuss this further with your midwife/doctor or a supervisor of midwives. When they are confident that you have made an informed decision, a plan will be made and included in your notes in order to inform everyone who may care for you in labour.
Of course you can change your mind at any time.
Where can I find further information?
National Institute for Clinical Excellence.
Royal College of Midwives Normal Birth Campaign.
If you would like to speak to a midwife about the information in this article, please contact your named community midwife. Alternatively a midwife on the labour ward will be happy to advise you.
Royal Sussex County Hospital
Eastern Road
Brighton
BN2 5BE
Telephone 01273 696955, Extension 4373
Princess Royal Hospital
Lewes Road
Haywards Heath
RH18 4EX
Telephone 01444 441881, Extension 8488.
This information is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
This article is intended for patients receiving care in Brighton & Hove or Haywards Heath.
Publication Date: September 2014
Review Date: December 2022


