DMMO lesser toe correction
Download and print as a PDF
DownloadWhat is DMMO?
Distal metatarsal minimally invasive osteotomy (DMMO) is the surgical technique used for correcting claw toes and metatarsalgia (pain in the forefoot, most commonly in the ball of the foot). Claw toes can develop in any toe except the big one. A muscle imbalance causes ligaments and tendons to tighten making the toes curl inward.
Changing your footwear and wearing specially made splints can help with toe shape and comfort. Surgical intervention is often considered once non-surgical treatments are no longer helping you with pain, and daily activities become difficult to manage.
What happens during surgery?
The aim of this surgery is to shorten and elevate the toes through correcting the alignment.
The minimally invasive technique for DMMO involves a 3 mm cut being made at the base of each relevant metatarsal (the bones in your foot). An osteotomy is made (the cutting of a bone to re shape it through healing) which will shorten and elevate the toes and is done under x-ray guidance. Sutures (stitches) are not required as the ligaments are left intact. A post-operative bandage is applied in theatre.
There are a number of reasons why a minimally invasive technique is preferred by some surgeons; a possible reduction in the risk of infection and pain, a quicker recovery period due to reduced tissue trauma and a reduction in joint stiffness.
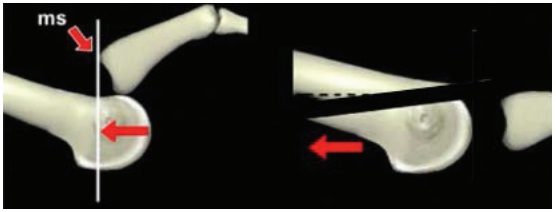
Side view of osteotomy made during surgery
What happens after surgery?
You will have your surgery at the Sussex Orthopaedic Treatment Centre (SOTC). This is usually done as day case surgery using either; regional anaesthesia (regional nerve block) that numbs your leg, or a general anaesthetic.
After your surgery you will have a bandage on your foot. The aim of the bandage is to support your toes in their new position whilst the bones in your foot are healing. This will be changed at your 2 and 6 weeks follow up appointments.
The recovery staff will give you an orthopaedic flat shoe to protect your foot. You will be wearing the flat shoe for 6 weeks at all times when walking.
You will able to put all your weight through your foot immediately after your surgery, and be given a pair of crutches to help with your walking. These are to be used for the first 2 weeks after your operation, then to be used as necessary. We would encourage you to discard the crutches by your 6 week follow up appointment.
During the first 2 weeks after your surgery we advise you to elevate your leg as high as you are able to and apply ice if required. Elevation and icing of the foot will help to reduce the swelling. The swelling can be expected to last for between for 3-6 months. Please walk regularly for short periods.
Immediately after surgery, you should no longer experience pain in the ball of the foot but could have pain in your forefoot for up to two weeks as this is where the osteotomies (the cutting of a bone to re shape it through healing) were made.
Two weeks after surgery
At 2 weeks you will have a post-operative wound check with a nurse who works in Mr Vernois’ team. Two weeks after surgery What happens after surgery?
Your bandage will be removed and the surgical wound/s assessed. The nurse will then re-apply your bandage.
Do not get this dressing wet in any way as this can cause complications to your surgical wound.
Six weeks after surgery
At your 6 week follow up appointment you will see a nurse from Mr Vernois’ team and have an x-ray taken.
Your dressing will be taken down and your surgical wound/s will be reviewed. We would expect these to be healed by this time. You will not need a further dressing at this stage.
The nurse will discard your orthopaedic flat shoe as the bones in your foot will have healed enough to walk on without it. Please bring suitable footwear with you to change into. A firm but pliable sole with forefoot coverage is recommended.
You will be shown exercises that will help you to loosen your toe joints and increase their range of movement.
You can start to drive and resume low impact sports after this appointment.
Three months after surgery
At this stage you will have an appointment with Mr Vernois. An x-ray of your foot will be taken and this will be reviewed. You will then be discharged from his care.
High impact sport can be resumed after this appointment.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information here is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.


