cholecystitis
Download and print as a PDF
DownloadWhat is Cholecystitis?
Cholecystitis
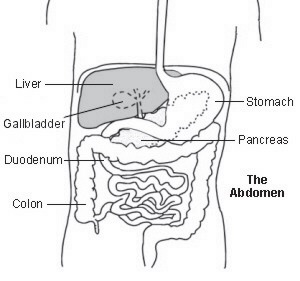
Cholecystitis is inflammation of the gallbladder. The gallbladder lies under the liver on the right side of the upper tummy (abdomen). It is like a pouch which comes off the main bile duct and fills with bile. Bile is a fluid made in the liver which helps to digest food, particularly fatty foods.
About one in three women, and one in six men, form gallstones at some stage in their life. Gallstones become more common with increasing age. The risk of forming gallstones increases with pregnancy, obesity, rapid weight loss, having a close relative with gallstones, diabetes and if you take certain medicines such as the contraceptive pill.
What are the causes of Cholecystitis?
Cholecystitis
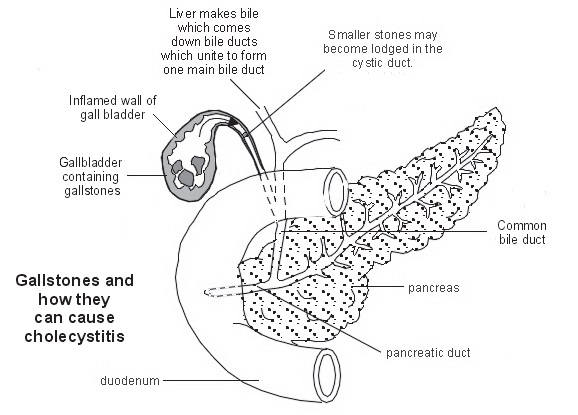
Gallstones occur when bile, which is normally fluid, forms stones. Gallstones commonly contain lumps of fatty (cholesterol-like) material that has solidified and hardened. Most people with gallstones do not have any symptoms or problems, and do not know they have them. Commonly, the stones simply stay in the gallbladder and cause no harm. However, in some people, gallstones can cause problems. In some people the stones can cause irritation to the Gallbladder resulting in infection, fever and pain.
If the stones move from the gallbladder into the cystic duct, the gallbladder attempts to ‘squeeze’ the stone out causing acute abdominal pain called biliary colic. The pain eases and goes if the gallstone is pushed out into the bile duct (and then usually out into the gut), or if it falls back into the gallbladder.
Obstructive jaundice can occur if a gallstone comes out of the gallbladder, but gets stuck in the bile duct. Bile then cannot pass into the gut, and so seeps into the bloodstream. This causes the whites of the eyes and dependent of the levels of bilirubin in the blood, the skin to become yellow. In these rare cases the stone needs to be removed via endoscopy or surgically.
How is Cholecyctitis diagnosed?
In many cases your symptoms, combined with tenderness in the upper right side of your tummy (abdomen), will alert the doctor that this is likely to be gallstones. Blood tests will be done to check your inflammatory markers and liver function. An ultrasound scan will visualise any potential stones. If the doctors are concerned that the stone is blocking a duct then a more intricate scan MRCP (MRI) may be required. The results of this will highlight the need to remove an obstructing stone via Endoscopy (ERCP). ERCP is a procedure that uses an endoscope and X-rays to look at the bile duct and the pancreatic duct. ERCP can also be used to remove gallstones or take small samples of tissue for analysis via a flexible telescope passed into the stomach and duodenum.
What is the treatment?
It is often best to leave gallstones alone if they cause few or no symptoms. If symptoms are problematic after fatty food, it makes sense to avoid that type of food.
If your blood results show you have signs of infection or you have a fever, antibiotics may be given alongside pain relief and fluids. It may require you to stay in hospital until the pain or infection settles.
An operation to remove the gallbladder is the usual treatment if you have symptoms caused by gallstones. This will usually be done at a later date (2-12 weeks) to ensure the inflammation has settled.
Keyhole surgery is now the most common way to remove a gallbladder. The medical term for this operation is laparoscopic cholecystectomy. It is called keyhole surgery, as only small cuts are needed in the tummy (abdomen) with small scars remaining afterwards. The operation is done with the aid of a special telescope that is pushed into the abdomen through one small cut. This allows the surgeon to see the gallbladder. Instruments pushed through another small cut are used to cut out and remove the gallbladder. Keyhole surgery is not suitable for all people. This will be an elective day surgery procedure.
Hospital stay
If your gallstones require you to remain in hospital for treatment then remember:
- Mobilise regularly to avoid any further complications including blood clots and chest infections.
- Try to stick to a low/no fat diet to avoid flare ups.
- The doctors may wish for you to wear anti-embolic stockings and receive an injection daily to help prevent formation of blood clots.
Contact details
Emergency Ambulatory Care Unit: Telephone: 01273 696955 Level 4 Extension 7591, Level 5 Extension 64002.
Further reading and references: www.patient.co.uk.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information here is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Review Date: November 2022


