bartholins cyst
Download and print as a PDF
Download- What is a Bartholin’s cyst and/or abscess?
- What are the signs and symptoms of a Bartholin’s cyst and abscess?
- Who gets a Bartholin cyst/abscess?
- How is a Bartholin’s cyst and/or abscess treated?
- What does the outpatient procedure involve?
- What does this catheter mean for my normal activities?
- What follow up will I get?
- What to expect before the operation?
- What does the operation involve?
- What are the risks?
- What can I expect after the operation?
- What about going home?
- What alternatives are there?
- Who can I contact with any concerns or questions?
What is a Bartholin’s cyst and/or abscess?
Bartholin glands can be found on either side of the entrance to the vagina.
These glands produce and secrete mucus to help the vagina stay moist. Sometimes the ducts to these glands can become blocked causing swelling known as a cyst.
If the cyst becomes infected, an abscess forms filling with fluid/pus. It is not certain as to why these glands can become blocked.

What are the signs and symptoms of a Bartholin’s cyst and abscess?
A cyst/abscess size can vary from the size of a small pea up to the size of a golf ball. A Bartholin cyst can sometimes go unnoticed, but symptoms may include:
- A tender lump on one side of the vagina where the ducts are situated
- The area can look red and feel swollen and hot to touch
- Discomfort and/or pain is felt when pressure applied eg: sitting
or walking - You can experience pain during sexual intercourse
- Pus can begin to ooze from the area (abscess) and be foul smelling
- You may find it uncomfortable to pass urine (stinging sensation)
Who gets a Bartholin cyst/abscess?
1 in 50 (2%) females can develop a cyst or abscess for reasons which are unknown. Most commonly these women are sexually active and ages range between 20-30, but Bartholin’s cysts/abscesses can occur at any age of a woman.
How is a Bartholin’s cyst and/or abscess treated?
This can vary depending on the severity of your symptoms.
A doctor will diagnose whether you have a cyst or an abscess by assessing you; this is carried out by examining the area and asking you questions regarding your signs and symptoms.
Cyst
If the cyst is small and not causing much discomfort then the best course of treatment may be to leave it alone.
Soaking the area in warm water up to three times a day can help for relief purposes.
Antibiotics may be prescribed if the doctor feels the cyst could develop
into an abscess.
Abscess
If an abscess has developed then it will almost always need treatment
- Antibiotics
- A procedure to drain the abscess called WORD catheter
- A minor operation.
What does the outpatient procedure involve?
If you are aged under 40 years old and the doctor suggests this then a catheter is inserted into the abscess/cyst, this drains the fluid in order to stop the cyst or abscess coming back. The procedure can be done in the Gynaecology Assessment Unit on Level 11 and requires no preparation.
A small amount of local anaesthetic is injected via a tiny needle into the cyst or abscess. A hole is made to drain the fluid away. A short rubber tube, called a catheter, is placed inside the gland and the balloon at the end of the catheter is inflated with saline in order to keep the catheter in place. The catheter remains in the gland so that the hole stays open permanently, even when the catheter is removed. The catheter is designed to stay in for up to 4-6 weeks, but sometimes falls out before this. If the catheter falls out in the first 2 weeks, please contact L11-Gynae Assessment Unit (GAU) for advice/re-assessment.
What does this catheter mean for my normal activities?
The catheter should not interfere with usual activities. Most women can go about their work and exercise with no problem. For convenience, the end of the catheter can be tucked inside the vagina. It is recommended to avoid tampon insertion or douching
What follow up will I get?
You will be asked to come back in 4-6 weeks for removal of the WORD catheter. If the catheter falls out prior to this, please contact GAU.
What to expect before the operation?
This minor operation is not usually carried out the same day that you have been seen by a doctor. Depending on urgency you will either be booked onto the emergency fast track theatre list at the Royal Sussex County Hospital usually within 24 hours. Alternatively you will be placed onto an elective theatre list at either RSCH, Lewes Victoria Hospital or the Princess Royal Hospital depending on availability. We will inform you when to return to the hospital for your operation.
Ideally you will be admitted, have your surgery and return home the same day. If, due to other very unwell patients requiring surgery, your operation cannot be done before midnight on the day of your admission we will cancel your operation until the next day. Unless an operation is life threatening we do not operate after midnight due to safety issues.
On the day of your admission please do not eat anything 6 hours before your admission time this includes sweets and chewing gum. Drink water only for 2 hours before your admission time.
Please note the following:
- If you are a smoker we strongly recommend that you do not smoke at all on the day before and the morning of your operation or for 48 hours after your operation
- Please bring in with you any medication that you usually take
- Do not bring in valuables or money except for some change
for the Patientline TV and phone - Do not wear make-up, nail varnish or jewellery
- Please remove your contact lenses.
A pre-op assessment will be undertaken by the ward staff nurse on duty before you go home. They will discuss your hospital admission and the operation you have been booked for.
Please do let us know about any concerns you have or if you think there is any information you think we should know about that will make your stay with us more comfortable.
You will need to make arrangements for your family, children or any other commitments that you have prior to coming into hospital and to cover the length of your recovery.
On your admission day you will see an anaesthetist and the doctor performing the surgery before going into theatre. It is not unusual to feel anxious; the nursing staff will gladly discuss how you are feeling and talk through your emotions.
What does the operation involve?
The main aim of the operation is to drain any fluid or pus causing discomfort to you and to prevent the cyst/abscess from reoccurring.
This operation is called ‘marsupialisation’ and is performed under general anaesthetic (meaning you are asleep). The doctors make a small incision (cut) to the problematic area allowing the pus/fluid to drain free. This should only take the doctors 10-15 minutes to complete.
During surgery the doctors may insert a small piece of gauze into the incision acting as a wick to aid the pus/fluid to drain without the wound healing too quickly, risking the chances of reoccurrence.
What are the risks?
As with having any operation, a marsupialisation comes with risks. The main risks associated are:
- Post-operative infection of the wound
- Reoccurrence cannot be excluded (2-25% reoccurrence rate)
- Patency and function of the duct operated on might not be fully
restored this affecting 20% of cases.
In order for you to make an informed choice about your procedure, please ask one of the doctors or nurses if you have any questions about the marsupialisation before signing the consent form.
What can I expect after the operation?
After having a general anaesthetic you may experience episodes of pain and/or nausea this is very common. Please let the nursing staff know and they will assess you and take appropriate action. Your nurse will be checking your blood pressure, pulse, breathing and temperature and monitoring the wound for any oozing/bleeding.
Once you are fully awake you will be able to start drinking and eating.
What about going home?
Having this operation as a day case procedure you should be able to go home within two–four hours after your operation.
Before you go home you need to have had something to eat, be able to walk around OK and have passed urine.
To allow the hospital to discharge you home you need to have a responsible adult to stay with you for 24 hours and have transport home. You will not be able to drive yourself home or take public transport.
The anaesthetic is short-lasting. You should not have, or suffer from, any after-effects for more than one day after the procedure. During the first 24 hours you may feel more sleepy than usual and your judgement
may be impaired.
After a general anaesthetic your co-ordination and logical thinking may be temporarily affected due to the drugs.
For your own safety it is important to follow these instructions:
- You must not drive yourself home and should not drive for 48 hours
- You must not drink alcohol
- You must not operate machinery or appliances that may cause harm
- You should not make any vital decisions or sign legal documents.
If you have a gauze wick in the wound after your operation this must be removed prior to you going home.
You will be given pain killers to go home with to take regularly if you feeling discomfort. You should be back to normal activities of daily living within 3-4 days but ensure plenty of rest.
It is important to keep the vaginal area clean and you are advised to have daily baths, avoid tight fitting clothes and wear sanitary towels if the wound is oozing still. Wound oozing is normal and will begin to ease off with time when the wound is healing.
Avoid sexual intercourse until the discharge has stopped and you are pain free
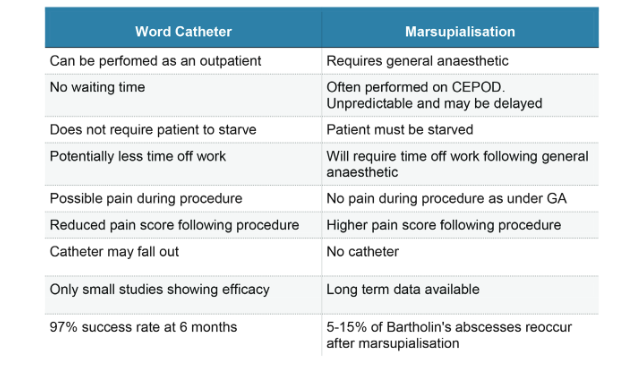
What alternatives are there?
- Sitting in a warm bath for three or four times a day, may encourage a Bartholin’s cyst to burst naturally.
- Performing the marsupialisation under local anaesthetic (numbing the area) which you will be awake for.
Your doctor should explain all alternatives to you prior to having the proposed procedure and explain why that chosen option is necessary letting you have an open and informed choice regarding your care and management.
Who can I contact with any concerns or questions?
If you have any problems or are worried, please do not hesitate to contact us on the gynaecology ward:
Royal Sussex County Hospital
Level 11 Telephone: 01273 523191
Princess Royal Hospital
Horsted Keynes Telephone: 01444 441881 Ext. 5686
This information sheet has been produced by the Gynaecology Ward Sisters Samantha Backley and Samantha Nair.
References/useful links
1. Patient UK. (2010). Information Leaflets: Bartholin’s Cyst and Abscess.
2. Patient UK. (2010). Professional Reference: Bartholin’s Cyst.
3. NICE (2009) Balloon catheter insertion for Bartholins’ Cyst or Abscess
4. BSUH management of Bartholin’s Cyst (2015).
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Review Date: September 2022


