appendicitis
Download and print as a PDF
DownloadAppendicitis
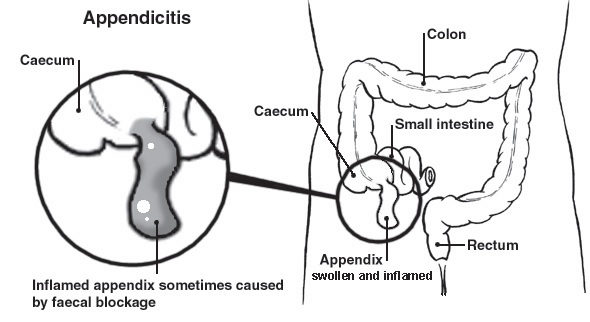
Appendicitis
Appendicitis means inflammation of the appendix. The appendix is a small pouch that comes off the gut wall. Appendicitis is common. Typical symptoms include abdominal pain and vomiting that gradually get worse over 6-24 hours. Some people have less typical symptoms. An operation to remove the inflamed appendix is usually done before it perforates (bursts). A perforated appendix is serious.
What is appendicitis?
Appendicitis means inflammation of the appendix. The inflamed appendix becomes infected with bacteria (germs) from the intestine. The inflamed appendix gradually swells and fills with pus. Eventually, if not treated, the swollen appendix might perforate (burst). This is very serious, as the contents of the intestine then spill into the abdominal cavity. This can cause a serious infection of the membrane that lines the abdomen (peritonitis), or an abscess in the abdomen. So, if appendicitis is suspected, early treatment is best before it bursts.
Who gets appendicitis?
Appendicitis is common and can affect anyone of any age. Teenagers and young adults are the most commonly affected. About 6 in 100 people in the UK have appendicitis at some time in their life. Appendicitis is the cause of the most common abdominal surgical emergency admission to hospital in the UK. It is slightly more common in men than in women. The appendix is a small dead end pouch, like a little tube, that comes off the caecum. The caecum is the first part of the large intestine (large bowel) just before the colon. The appendix is normally about 5-10 cm long and quite thin. The appendix appears to have no function and the reason it is there is a bit of a mystery.
What are the symptoms?
Pain in the abdomen (tummy pain) is usually the main symptom. Commonly, the pain starts in the middle of the abdomen. The pain normally develops quickly, over an hour or so. Over the next few hours the pain typically travels to the lower right-hand side of the abdomen. This is over where the appendix normally lies.
Typically the pain becomes worse and worse over 6-24 hours. The pain may become severe. The pain tends to be sharper if you cough or make any jarring movements. The pain may ease a bit if you pull your knees up towards your chest. The lower abdomen is usually tender, particularly in the lower right-hand side.
Other symptoms that may occur include the following:
- Feeling sick and being off food is typical. You may vomit.
- Fever and generally feeling unwell.
- Constipation or diarrhoea may occur.
- Frequent passing of urine may develop.
This is thought to be due to the inflammation irritating the nearby ureter (the tube between the kidney and bladder).
In some cases, the symptoms are not so typical. For example, in some cases the pain may develop more slowly and start in the lower left-hand side or centre of the abdomen. Also, the pain may not become severe until the appendix perforates. The site of the pain may not be typical if the appendix lies in an unusual place.
A doctor may diagnose appendicitis quite easily if you have the typical symptoms. However, as described above, not everyone has typical symptoms. Sometimes it is difficult for doctors to be sure that appendicitis is the cause of the symptoms A blood test will be performed to check the inflammatory markers which can be an indicator of appendicitis. An ultrasound scan or a CT scan may help to clarify the cause of the symptoms in some cases. Sometimes a surgeon advises to wait and see for a few hours or so while you are being monitored in hospital. This allows some time to see if your symptoms progress to a more definite diagnosis, or even if they change or go away.
Treatment
Surgery is commonly done by a keyhole (laparoscopy) operation, as the recovery is quicker compared to having an open operation. The keyhole operation is performed through three tiny cuts, the largest of which is only around 1.5 cm in size. Laparoscopy is a procedure to look inside your abdomen by using a laparoscope. A laparoscope is like a thin telescope with a light source. It is used to light up and magnify the structures inside the abdomen.
Post operatively
You may feel a little sore around the incisions. You may have some pain in your shoulder tip. This is caused by the gas which had been pumped inside during the operation to make it easier for the surgeons to view your organs. This gas irritates the diaphragm which has the same nerve supply as the shoulder tip. This pain soon passes off and mobilising can help relieve it earlier. The length of time to recover can vary depending on the condition of the appendix; however you will hopefully be able to leave hospital 6 -12 hours after the operation. You will be given simple pain relief to take home, and may need up to a week off work. You are not safe to drive until you can do an emergency stop (average 5 days), though best to check with your insurer.
Dressings will be on the laparoscopy sites that can be left off as soon as they are dry (average 2 days), there is not normally stitches in place unless you have been advised so. You can shower as normal though avoid baths and heavy lifting for 7 days.
If the appendix is very infected, perforated or has dead tissue a larger incision may be required to ensure the area is washed out. This may require a slightly longer stay in hospital as intravenous antibiotics and dressing changes to monitor the wound may be needed. It is still essential to mobilise early post operatively as this reduces any further complications including blood clots and chest infections.
Before Surgery
1. You will be Nil by Mouth; this means no food or drink (including chewing gum) to be consumed 6 hours prior to going to theatre. You will be able to drink clear fluids (water) up until 2 hours before theatre. A drip may be connected to a cannula in your arm or hand to keep you from getting de-hydrated.
2. You will be dressed in a theatre gown and surgical stockings (to prevent blood clots) to prepare you for theatre. Please remove all jewellery, make-up and nail varnish.
3. You will be place on an emergency surgery list. The nurses will not be able to give you an exact time as other emergencies may be prioritised before you depending on their severity.
Contact details for the Emergency Ambulatory Care Unit.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information here is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Review Date: October 2022


